Bad breath? Bleeding gum? Signs you may have Gum Disease
What Is Gum Disease?
Gums are the supportive tissues around your teeth, keeping them secure. Gum disease, also known as periodontal disease or periodontitis by dentists, occurs when these tissues become infected. It begins with the growth of bacteria in the mouth, which thrives when oral hygiene, including brushing and flossing, is inadequate. Left untreated, gum disease can lead to symptoms like swelling, redness, discomfort, and eventually tooth loss.
Nearly half of adults aged 30 and above show indications of gum disease, with around 9% experiencing severe cases.
Gingivitis vs. Periodontitis
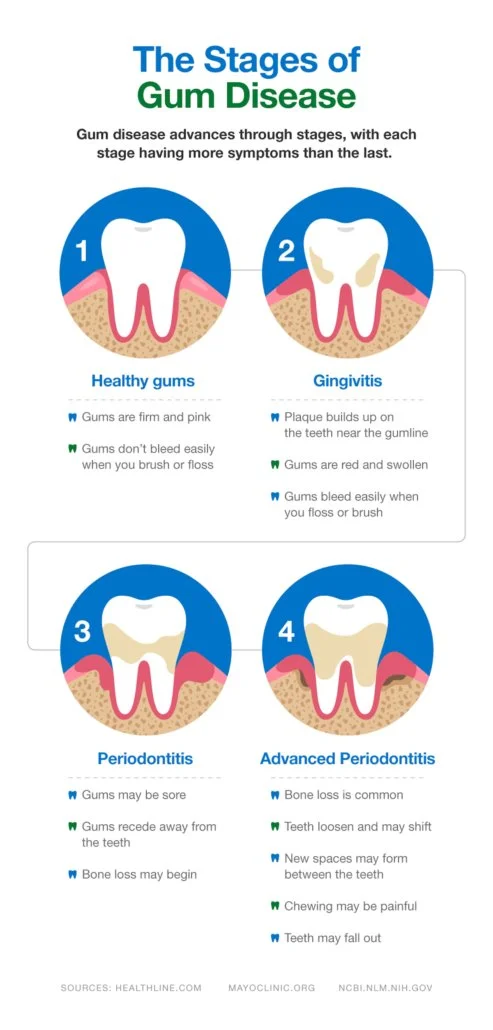
Gingivitis is characterized by swollen, red, and bleeding gums surrounding your teeth. It represents an early stage of gum disease that can progress to periodontitis if left untreated.
When oral hygiene lapses—skipping brushing, flossing, and rinsing with mouthwash—bacteria and food residue form a sticky film known as plaque. This substance releases acids that attack the enamel, the outer protective layer of teeth, leading to decay. If not removed within 72 hours, plaque hardens into tartar along the gumline, making thorough cleaning difficult and causing irritation and inflammation of the gums, resulting in gingivitis.
Regular brushing, flossing, regular dental checkups and cleanings can help prevent or reverse gingivitis, ensuring optimal oral health.
Causes
Plaque is the primary cause of gum disease, with gingivitis developing as follows:
After consuming sweet or starchy foods, bacteria accumulate on your teeth. Inadequate brushing and flossing allow these bacteria to form plaque, a sticky film on your teeth. Plaque hardens into tartar along the gumline, trapping more bacteria and worsening tooth damage.
As a result, gums become irritated, red, and swollen, often bleeding during brushing. Over time, gums may recede and form pockets where bacteria, plaque, and tartar accumulate, leading to infection. This infection progressively breaks down the bone and connective tissue supporting teeth, potentially causing them to loosen and fall out. Gum disease is the leading cause of adult tooth loss.
Several factors increase the risk of gum disease:
- Hormonal changes during pregnancy, puberty, menopause, and menstruation make gums more sensitive and prone to gingivitis.
- Diseases like cancer, HIV, and diabetes heighten the risk of infections, including periodontal disease.
- Certain medications reduce saliva production, which protects teeth and gums. These include drugs for seizures and angina.
- Smoking impairs gum tissue repair.
- Poor oral hygiene practices, such as infrequent brushing and flossing, contribute to gingivitis.
- A family history of dental issues increases susceptibility to gum disease.
Symptoms
The typical signs of gum disease include:
- Bleeding gums during brushing
- Redness and swelling of the gums (healthy gums should be pink and firm)
- Gum pain or tenderness
- Persistent bad breath or an unpleasant taste in the mouth
- Discomfort when chewing
- Tooth sensitivity
- Presence of pus between teeth
- Receding gums, where gums pull away from teeth
- Formation of deep pockets between teeth and gums
- Loose teeth or teeth that may fall out
- Visible spaces between teeth resembling black triangles
- Changes in how teeth fit together when biting
Gum disease can sometimes affect specific teeth, such as molars, in certain individuals. Only a dentist or periodontist can accurately diagnose gum disease.
Is periodontal disease contagious?
Yes, gum disease can be caused by bacteria. These bacteria can spread through saliva, such as when kissing someone with gum disease or sharing utensils with them. However, it's important to note that you cannot catch periodontal disease solely from being in close proximity to someone who has it.
Diagnosis
Gum disease is diagnosed by a dentist who assesses specific symptoms during a dental examination, including:
- Bleeding and swollen gums
- Formation of pockets between gums and teeth
- Receding gums
- Changes in your bite
- Loose teeth
If necessary, your dentist may refer you to a periodontist, a specialist in gum health, for further evaluation and treatment. During the examination, the dentist or periodontist uses a periodontal probe, a small ruler, to measure the depth of pockets around your teeth. Deeper pockets indicate more significant bone loss. Dental X-rays are also used to provide a clearer view of any bone loss that may have occurred.
Treatment
Nonsurgical treatments for mild periodontitis aim to address gum disease without invasive procedures:
- **Scaling**: This deep cleaning removes tartar, plaque, and bacteria from below the gumline using instruments, lasers, or sound waves.
- **Root planing**: Smoothing the tooth root's surface helps prevent bacteria and plaque buildup and encourages gum reattachment.
- **Antibiotic treatments**: Mouth rinses, gels, or pills eliminate infection-causing bacteria.
If you have advanced periodontitis, you may need once of these surgical procedures: Flap surgery, soft tissue grafts, bone grafting, guided tissue regeneration (GTR),.etc. These treatments are tailored to the severity of gum disease and aim to restore oral health and prevent further deterioration.
Can Gum Disease Be Reversed?
Early treatment of gum disease can reverse its progression. Once bone loss around the teeth occurs, however, it is irreversible. Nonetheless, effective treatment and consistent oral hygiene practices can help slow down or halt the advancement of gum disease. This underscores the importance of early detection and proactive management to preserve oral health and prevent further complications.
Watson, S. (2024, February 21). Gingivitis and periodontal disease (GUM disease). WebMD. https://www.webmd.com/oral-health/gingivitis-periodontal-disease